Tennessee is in the midst of an opioid crisis. In 2024, the state had the highest rate of opioid use disorder diagnoses in the nation, affecting 1,447 out of every 100,000 insured patients. In 2025, the Substance Abuse and Mental Health Services Administration (SAMHSA) reported that an estimated 68,000 Tennessee residents misused prescription opioids or heroin, highlighting the urgent need for professional care, especially in Memphis and Shelby County, where families are seeking help for loved ones.
Opioid use disorder rewires the brain’s reward system, making it difficult to think clearly, manage stress, or control impulses. It often begins with a prescription after surgery and gradually takes hold as the body develops tolerance, requiring higher or more frequent doses, and physical dependence, leading to withdrawal symptoms if use stops.
Memphis Detox in Memphis, Tennessee, provides medically supervised opioid detox and individualized treatment to safely manage withdrawal and lay the foundation for long-term recovery.
What is Opioid Use Disorder (OUD)?
Opioid use disorder (OUD), defined in the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), is a chronic brain condition that alters reward and decision-making systems, making it difficult to manage stress, control impulses, or stop using opioids despite harmful consequences. Often starting with prescription pain medication, OUD can quickly progress as the body develops tolerance and dependence, leading to intense withdrawal and strong cravings.
When opioids are reduced or discontinued, individuals can experience intense withdrawal, including nausea, anxiety, and muscle aches, along with powerful cravings driven by changes in brain chemistry. An OUD causes compulsive use despite negative impacts on health, relationships, or daily life. Seeking a professional assessment is the safest first step toward recovery.
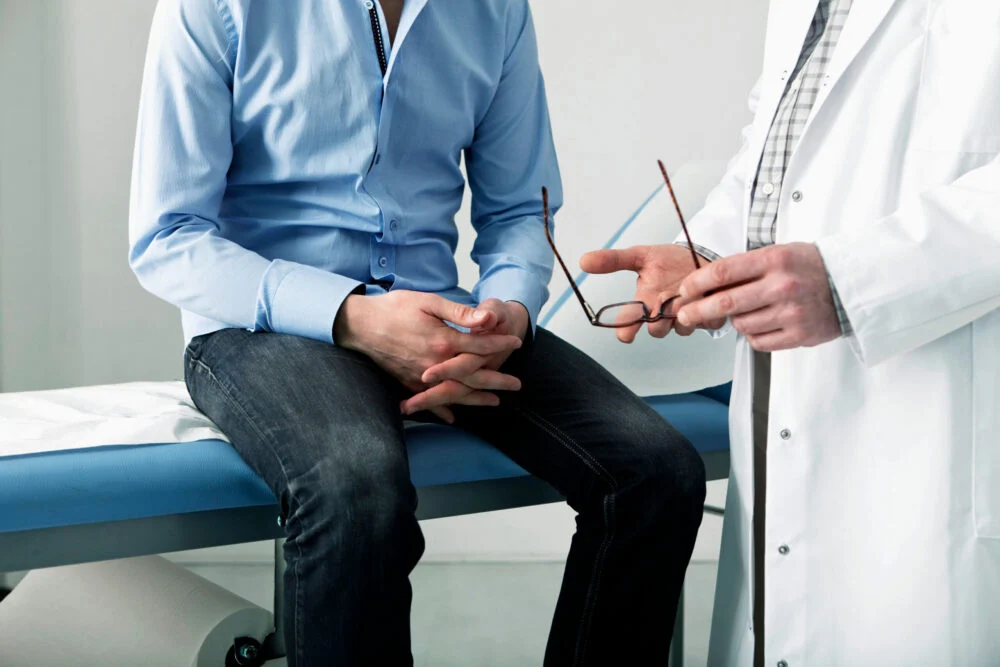

Types of Opioids Commonly Abused
Opioids that are commonly abused fall into three main categories: prescription painkillers, heroin, and synthetic opioids. While some begin as legitimate medical treatments for pain, all opioids carry a high risk for misuse due to their powerful effects on the brain’s reward system.
Synthetic opioids are among the most dangerous substances currently in circulation. Fentanyl is up to 50–100 times more potent than morphine and is frequently mixed into heroin or counterfeit pills without a person’s knowledge, significantly increasing overdose risk.
Regardless of the type, all opioids affect the same receptors in the brain, slow breathing, and can lead to tolerance, dependence, addiction, and potentially fatal overdose.
Prescription misuse often begins unintentionally, such as taking an extra pill for breakthrough pain, but repeated use can quickly lead to tolerance, escalating doses, and physical dependence. Opioids are often a person’s first exposure to this class of drugs. Medications such as oxycodone (OxyContin, Percocet), hydrocodone (Vicodin), morphine, and codeine are highly effective for treating moderate to severe pain, but they also carry a strong potential for misuse. When taken in higher doses or in ways not prescribed, they can produce feelings of euphoria in addition to pain relief.
In Tennessee, the number of opioid prescriptions has historically exceeded the state’s population, increasing availability and risk for misuse. According to the Tennessee Department of Mental Health and Substance Abuse Services, an estimated 70,000 residents misuse prescription opioids in Memphis and Shelby County.
Heroin is an illegal opioid derived from morphine that acts rapidly and produces an intense euphoric effect, increasing its addiction potential. When prescription opioids become too expensive, harder to obtain, or are discontinued, some individuals transition to heroin because it is often cheaper and more accessible. This shift significantly raises overdose risk, making timely heroin addiction treatment critical.
Heroin’s potency can vary widely, which increases the danger of accidental overdose. Today, illicitly manufactured fentanyl poses the greatest threat. Fentanyl is frequently mixed into heroin, other street drugs, or pressed into counterfeit pills, often without the user’s knowledge, dramatically increasing the likelihood of fatal respiratory depression.
How Do Opioids Affect the Brain and Body?
Opioids affect the brain and body by binding to opioid receptors that regulate pain, reward, mood, and breathing. Medications like morphine, oxycodone, heroin, and fentanyl reduce pain by blocking pain signals in the brain and spinal cord. At the same time, they trigger the release of dopamine in the brain’s reward system, creating feelings of relaxation or euphoria.
Because opioids slow the central nervous system, they can cause drowsiness, slowed thinking, and impaired coordination. They also suppress breathing by acting on the brainstem, which is why high doses can lead to respiratory depression and overdose.
In the body, short-term effects may include nausea, constipation, itching, slowed heart rate, and pinpoint pupils. With repeated use, the brain adapts, leading to tolerance (needing more to feel the same effects) and physical dependence. When someone stops taking opioids, withdrawal symptoms like muscle aches, anxiety, sweating, nausea, and intense cravings can occur.
Over time, opioids can alter decision-making and stress-response systems in the brain, increasing the risk of addiction. These changes help explain why opioid use can shift from voluntary to compulsive and why professional treatment is often needed for recovery.


Side Effects of Opioid Abuse
Opioid abuse affects both the body and brain, producing a wide range of short- and long-term side effects. In the short term, users may experience drowsiness, nausea, constipation, slowed breathing, impaired coordination, and euphoria. Chronic use can lead to tolerance (needing higher doses for the same effect), physical dependence, and addiction, along with more serious health issues such as liver damage, hormonal imbalances, weakened immunity, and increased risk of infections.
Abuse also significantly impacts mental health, causing anxiety, depression, mood swings, and impaired decision-making. The most dangerous side effect is respiratory depression, which can lead to overdose and death, especially when opioids are combined with alcohol or other depressants. Long-term misuse can also increase pain sensitivity (opioid-induced hyperalgesia) and disrupt daily functioning, relationships, and work life.
For individuals struggling with these effects, professional treatment at a facility like Memphis Detox in Memphis, TN, can provide medical supervision and supportive care to safely manage withdrawal and begin recovery.
Chronic opioid use can damage nearly every system in the body, with the most immediate and serious risk being respiratory depression, which can slow breathing to a fatal level. Long-term use can also lead to cardiovascular strain, including collapsed veins and heart infections like endocarditis, particularly in individuals who inject drugs. Gastrointestinal complications such as chronic constipation, nausea, and abdominal pain are common, while liver damage is a concern, especially when opioids are combined with alcohol or acetaminophen. Additionally, sharing injection equipment significantly raises the risk of infectious diseases such as HIV and hepatitis C, further endangering overall health.
Opioids flood the brain with dopamine, producing a temporary high, but with repeated use, the brain reduces its own dopamine production. Over time, this can lead to anhedonia, a state where nothing feels enjoyable. Opioid abuse also worsens mental health, often increasing anxiety and depression, and can cause cognitive decline, including difficulties with memory, concentration, and decision-making. Socially, relationships often suffer as the compulsion to obtain and use the drug takes priority, leading to isolation and social withdrawal.
Opioid Addiction Treatment at Memphis Detox
There’s no single treatment that works for everyone. The appropriate level of care, often considered as inpatient versus outpatient rehab, depends on factors such as addiction severity, substances used, and medical history. Medical detox provides a safe, supervised way to manage withdrawal symptoms, which for opioids can be both physically painful and mentally exhausting, typically peaking within the first few days.
At Memphis Detox, our clinical team offers 24/7 monitoring to respond immediately to any complications, medication-assisted symptom management to ease nausea, body aches, insomnia, and anxiety, and stabilization to prepare both body and mind for the next phase of recovery. Because detox alone rarely leads to lasting sobriety, transitioning into a structured treatment program afterward is critical for long-term success.
Medical detox provides a safe, supervised way to manage withdrawal symptoms, which for opioids can be both physically painful and mentally exhausting, typically peaking within the first few days. At Memphis Detox, our clinical team offers 24/7 monitoring to respond immediately to any complications, medication-assisted symptom management to ease nausea, body aches, insomnia, and anxiety, and stabilization to prepare both body and mind for the next phase of recovery. Detox is not a cure for addiction and rarely leads to lasting sobriety on its own. It is the first step in the recovery process, preparing individuals to transition into a structured treatment program, which is critical for achieving long-term success.
Medication-assisted treatment (MAT) combines FDA-approved medications with counseling to treat opioid use disorder by stabilizing brain chemistry, reducing cravings, and blocking the euphoric effects of opioids. Using medication in recovery is not replacing one addiction with another; it is a medical intervention that allows individuals to function, work, and rebuild relationships without constant withdrawal symptoms and cravings.
Common medications include buprenorphine and naltrexone, each serving a different role, depending on an individual’s specific needs and medical history. Buprenorphine is a partial opioid agonist that eases cravings and withdrawal symptoms with a lower risk of respiratory depression, making it a flexible and effective option for many patients. Naltrexone is an opioid antagonist that blocks opioid receptors and prevents opioids from producing a high, making it best suited for individuals who have completed detox and want additional protection against relapse.
Completing treatment is a major milestone, but recovery doesn’t end there. Addiction is a chronic condition that requires ongoing management, much like diabetes. Continued care reinforces the skills learned in treatment and provides support when challenges arise. Aftercare often includes outpatient counseling to address underlying issues, support groups like NA or SMART Recovery for peer accountability, and sober living environments for a safe transition if home isn’t supportive. Relapse doesn’t signal failure; it highlights the need to adjust the treatment plan.
Effective relapse prevention strategies focus on identifying triggers, building a support network, maintaining self-care through sleep, nutrition, and exercise, and keeping a structured daily routine. Additional aftercare components can include continued therapy, medication management if MAT is part of recovery, and actionable relapse prevention planning to maintain long-term sobriety and support a healthy, opioid-free life.
Many people with opioid use disorder also struggle with mental health conditions such as depression and anxiety. This is why addressing co-occurring disorders is essential; treating the addiction alone while ignoring underlying mental health issues often leads to relapse. Mental health challenges can contribute to opioid use, while opioid use can worsen symptoms, as many individuals use opioids to self-medicate feelings of sadness, anxiety, or hopelessness.
At Memphis Detox, we use an integrated dual diagnosis treatment approach, simultaneously addressing mental health and substance use with a coordinated clinical team and structured addiction counseling. This integrated care includes a comprehensive evaluation to screen for mental health disorders, trauma-informed care to recognize and avoid re-traumatization, and therapeutic alignment to ensure treatment addresses how mental health symptoms interact with substance use triggers.
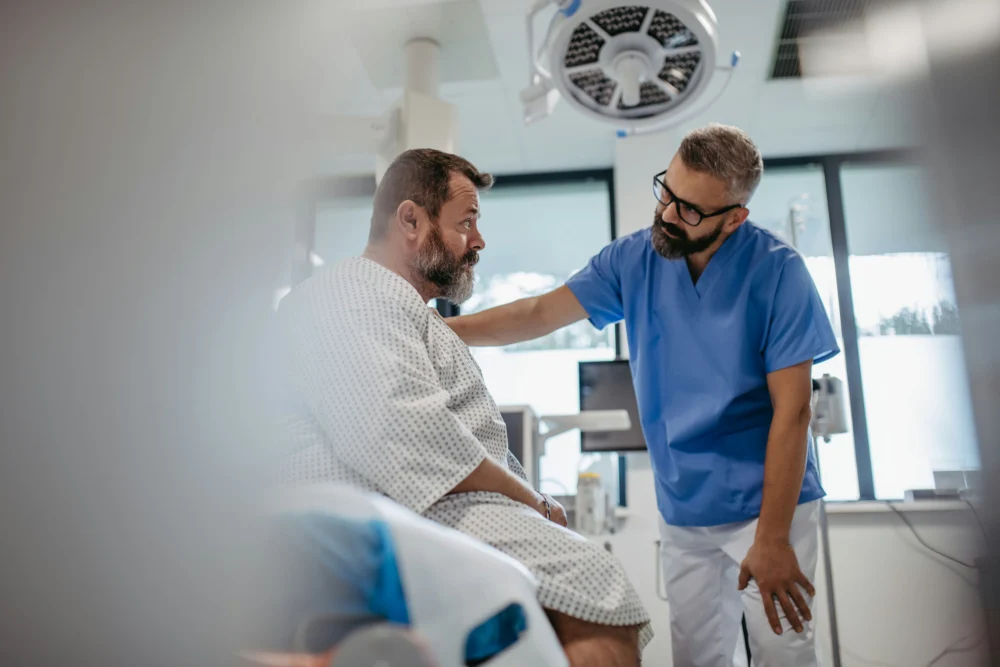

Choose Memphis Detox for Opioid Addiction Treatment
Entering treatment can be intimidating, but knowing what to expect can make the process easier. At Memphis Detox, our approach is transparent, respectful, and patient-centered. Upon arrival, you undergo a thorough assessment, which forms the foundation of your personalized treatment plan. Choosing the right facility is critical. Our team prioritizes safety, tailors care to each individual, and understands the unique challenges Memphis families face.
With Tennessee’s overdose rates rising, we provide local, accessible care so families can stay close and involved. Our accredited facility is staffed by experienced addiction medicine professionals who respect every person who walks through the door. We recognize the dangers present in Memphis, including fentanyl in the community and a shortage of accessible treatment, and offer a safe environment to safely withdraw and begin rebuilding a life free from opioids. Contact us today to take the first step toward recovery.


